Colorectal Cancer
Colorectal Cancer
CRC stage, Treatment, and Prognosis
CRC stage at diagnosis1
5-year relative survival rates by stage in the US
CRC, colorectal cancer; SEER, Surveillance, Epidemiology, and End Results.
1. National Cancer Institute. Cancer of the Colon and Rectum - Cancer Stat Facts. SEER 21 (Excluding IL) 2015–2021, All Races, Both Sexes by SEER Combined Summary Stage. Accessed August 2025. https://seer.cancer.gov/statfacts/html/colorect.html
| CRC stage2 | Treatment2 |
|---|---|
| Stage I |
|
| Stage II |
|
| Stage III |
|
| Stage IV |
|
2. American Cancer Society. Treatment of Colon Cancer by Stage. https://www.cancer.org/cancer/colon-rectal-cancer/treating/by-stage-colon.html (accessed August 2025).
Risk Factors and Health Disparities
Health Disparities in Colorectal Cancer (CRC)
General Risks1
- Family History: Individuals with a family history of CRC or adenomatous polyps are at increased risk
- Genetic Syndromes: Conditions such as Lynch syndrome (hereditary nonpolyposis colorectal cancer) and familial adenomatous polyposis (FAP) significantly elevate risk
- Inflammatory Bowel Disease (IBD): Chronic conditions like ulcerative colitis and Crohn’s disease increase the likelihood of developing CRC
- Diabetes: Type 2 Diabetes
High Risk Communities1
- American Indian and Alaska Native populations have the highest colorectal cancer rates and are often diagnosed at later stages
- According to the American Cancer Society: African Americans are about 20% more likely to get colorectal cancer and about 40% more likely to die from it
- States with the highest Colorectal cancer rates include: West Virginia, Kentucky, Arkansas, Mississippi and Louisiana
Contributors to Health Disparities2
- Limited Access: Challenges in accessing testing and quality healthcare services
- Lack of Awareness: Insufficient knowledge about available screening methods
- Genetic Factors: Unfamiliarity with family history related to colon cancer genetics
- Cultural Competence: Health systems may lack cultural awareness and trust with patients
- Research Participation: Low engagement in clinical research among affected communities
General Risk Factors for Developing Colon Cancer1
Inflammatory Bowel Disease
Genetic Syndromes
Family History
Type 2 Diabetes
These are AI generated images.
1.Infographic: Colorectal Cancer: Catching It Early | American Cancer Society. www.cancer.org. Accessed November 19, 2025. https://www.cancer.org/cancer/types/colon-rectal-cancer/prevention-infographic.html
2.Jackson CS, et al. J Gastrointest Oncol. 2015;7(Suppl 1):S32-S43.
Communities at Higher Risk of developing Colon Cancer
This is an AI generated image.
Early Onset Colorectal Cancer Rates Are Rising And Young Patients Are Diagnosed With More Advanced Disease in the US
Colon and Rectum Cancer
Recent Trends in SEER Age-Adjusted Incidence Rates1
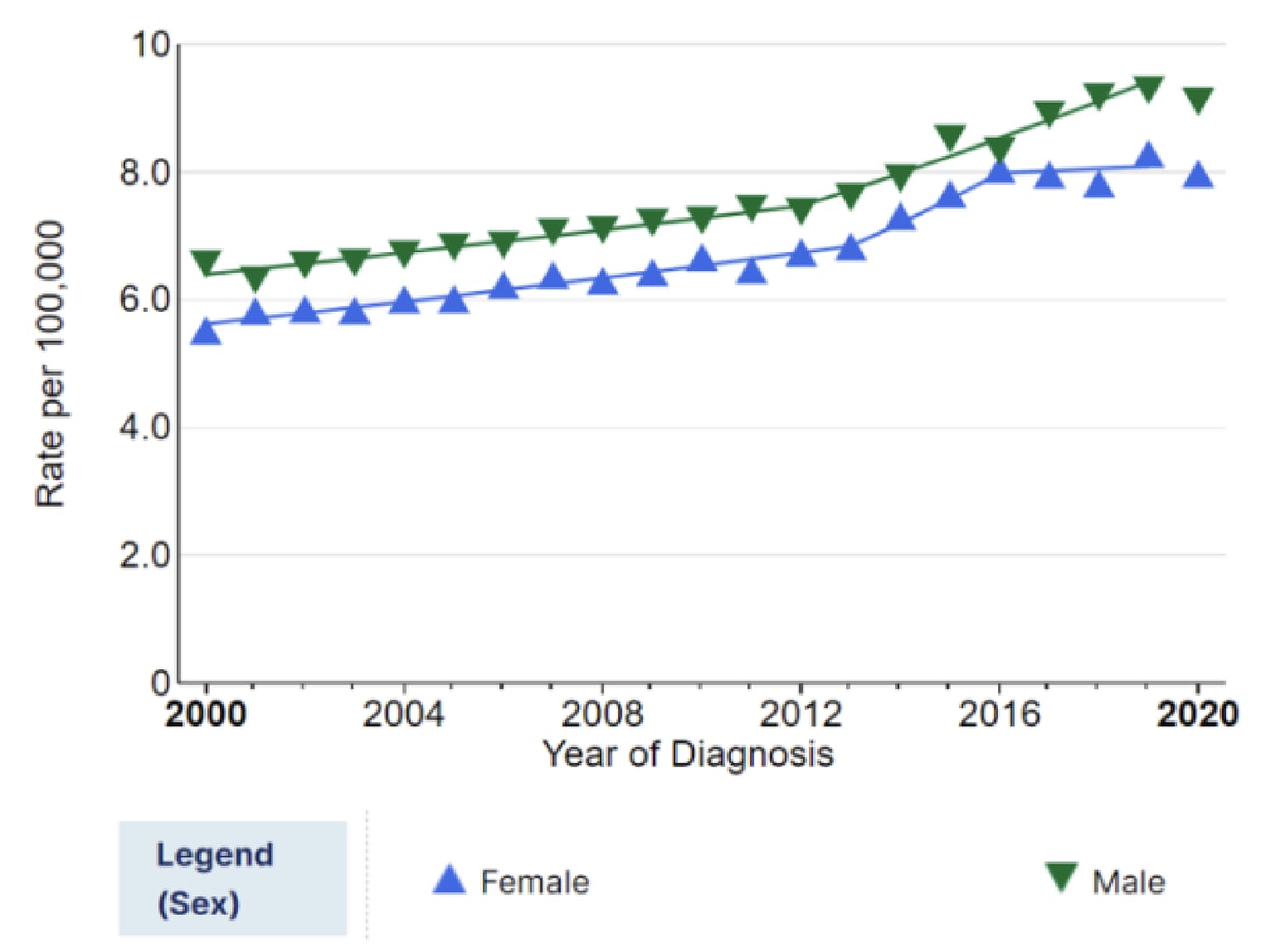
71% diagnosed with stage III/IV disease2
41% waited >6 months before seeking medical attention.2
67% saw 2 or more physicians prior to diagnosis.2
SEER, Surveillance, Epidemiology, and End Results Program.
1. SEER*Explorer Application. seer.cancer.gov. Accessed January 28, 2026. https://seer.cancer.gov/statistics-network/explorer/application.html?site=20&data_type=1&graph_type=2&compareBy=sex&chk_sex_3=3&chk_sex_2=2&rate_type=2&race=1&age_range=9&stage=101&advopt_precision=1&advopt_show_ci=on#resultsRegion0
2. Ng K. The Rise of Early-Onset Colorectal Cancer. Presented at Congressional Families Cancer Prevention Program 2019.
What You Need to Know About CRC Screening
Why should you get regular CRC screening?1
- To identify symptoms and risk for prevention of colorectal cancer early and initiate treatment that can prolong survival
- For example, colonoscopy screening can potentially prevent colorectal cancer by finding and removing precancerous polyps during the procedure
When should you get screened?2
- Average-risk individuals should begin regular screening at age 45.
- High-risk individuals should start screening before age 45 and do so more frequently.
- Healthy individuals should continue screening until age 75.
- Those aged 75-85 should consider screening based on personal preferences, life expectancy, health status, and past screening history.
- Individuals over 85 should discontinue screening.
Is screening covered by insurance?3
- Colorectal cancer screening is a preventive service that most health plans must cover
1. Screening for Colorectal Cancer. CDC. Published February 26, 2025. Accessed January 29, 2026. https://www.cdc.gov/colorectal-cancer/screening/
2. Colorectal Cancer - Early Detection, Diagnosis, and Staging. www.cancer.org. Published January 29, 2024. Accessed January 29, 2026. https://www.cancer.org/cancer/types/colon-rectal-cancer/detection-diagnosis-staging.html
3. Insurance Coverage for Colorectal Cancer Screening. www.cancer.org. Published March 20, 2023. Accessed February 28, 2024. https://www.cancer.org/cancer/types/colon-rectal-cancer/detection-diagnosis-staging/screening-coverage-laws.html
Types of Colorectal Cancer Screening Tests1-3
Colonoscopy* | Flexible Sigmoidoscopy | Virtual Colonoscopy | gFOBT | FIT* | Cologuard (FIT+DNA) | |
|---|---|---|---|---|---|---|
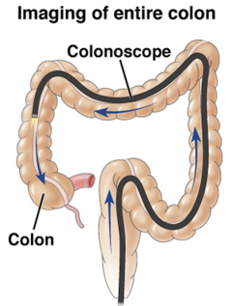 | 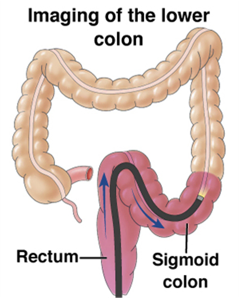 |  | 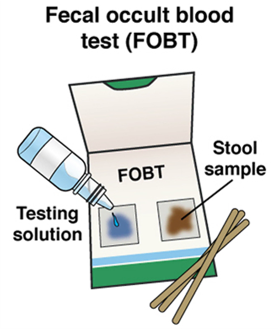 | 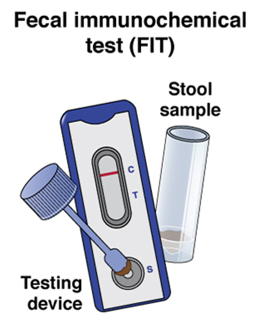 | 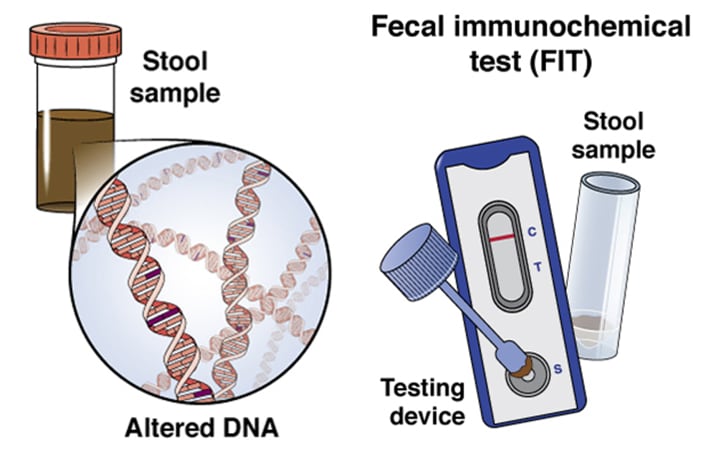 | |
What is it? | The rectum and entire colon are checked, and pre-cancerous polyps can be removed at the same time | Similar to a colonoscopy, but only the rectum and lower third of the colon are checked | The colon and rectum are examined using x-rays and CT imaging | The guaiac-based fecal occult blood test detects blood in the stool | The fecal immuno-chemical test uses antibodies to detect blood in the stool | Cologuard detects blood and altered DNA in the stool |
| Pre-screen requirements | Bowel prep is required | Bowel prep is required | Bowel prep is required | Dietary restrictions apply | No dietary restrictions or bowel prep | No dietary restrictions or bowel prep |
| Is it invasive? | Yes | Yes | No | No | No | No |
| Where is it performed? | Outpatient surgical center or hospital | Outpatient surgical center or hospital | Outpatient surgical center or hospital | At home and sent to lab | At home and sent to lab | At home and sent to lab |
| When should it be repeated? | Every 10 years, if normal | Every 5 years, if normal | Every 5 years, if normal | Every year | Every year | Every 3 years, if normal |
*American College of Gastroenterology recommended as primary screening modalities.
1. Screening for Colorectal Cancer. CDC. Published February 26, 2025. Accessed January 29, 2026. https://www.cdc.gov/colorectal-cancer/screening/
2. Shaukat A, et al. Am J Gastroenterol. 2021;116(3):458-479.
3. US Preventive Services Task Force, et al. JAMA. 2021;325(19):1965-1977.



